Prepare Your Child and Yourself
Use simple words your child will understand. Encourage your child to discuss feelings and ask questions about the upcoming experience but be careful not to force a discussion if your child does not seem ready. Be honest. If you do not know the answer to your child’s question, tell your child that you do not know, but that you will find out. Be aware that your visit may take a minimum of two to three hours. It is helpful to bring items to distract, entertain and comfort your child before and after sedation. Remain calm and take care of yourself. You will be able to provide better support for your child if you are rested and comfortable. The sedation process will be discussed during your entire visit, so there should be no surprises. Bring a spouse, a friend or a family member with you, but try to leave younger children at home and keep your party small to decrease stimulation in your child’s room. A second person will be very helpful during your journey home when your child is still groggy.
Picture Story
The Sedation Story was developed by Kalyani Raghavan, MBBS, MD, DCH, FAAP and Jennifer Twachtman-Bassett, MS, CCC-SLP with a grant from Autism Speaks. Click here to download a PDF version.









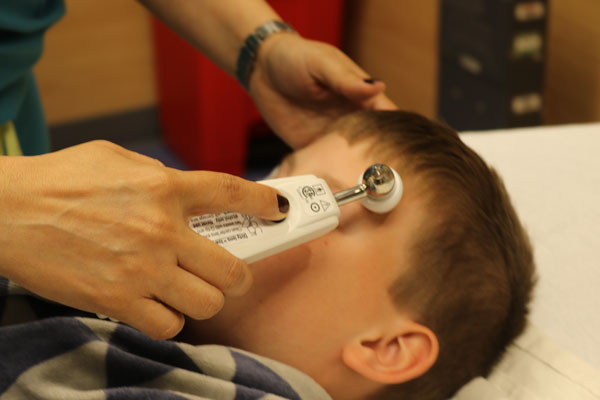
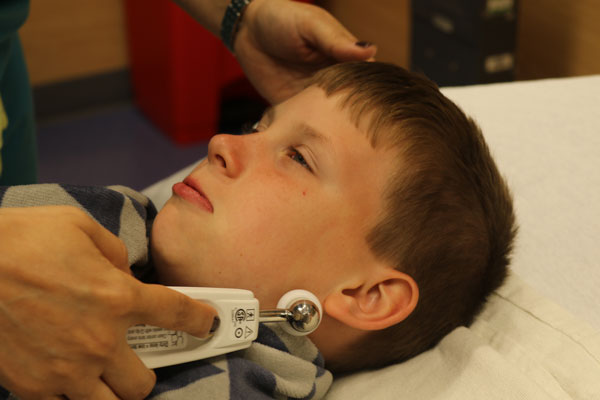
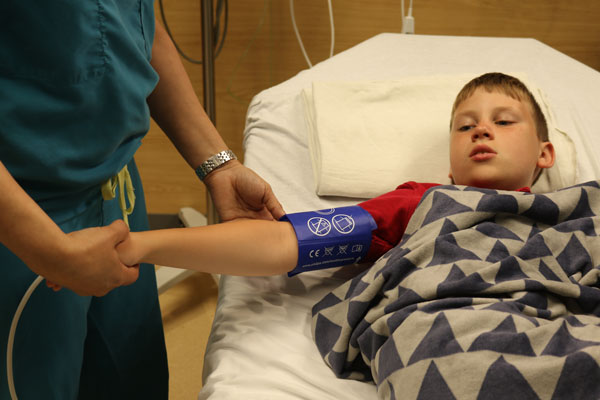

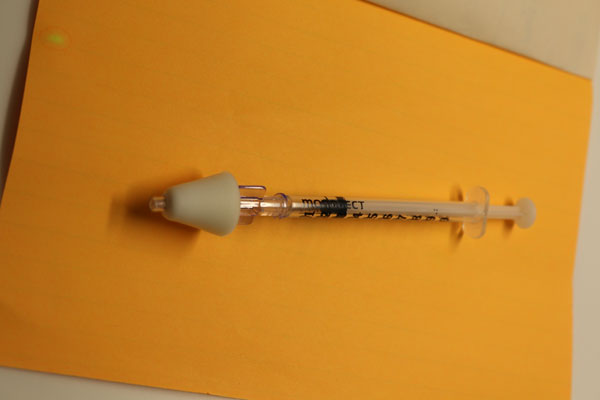
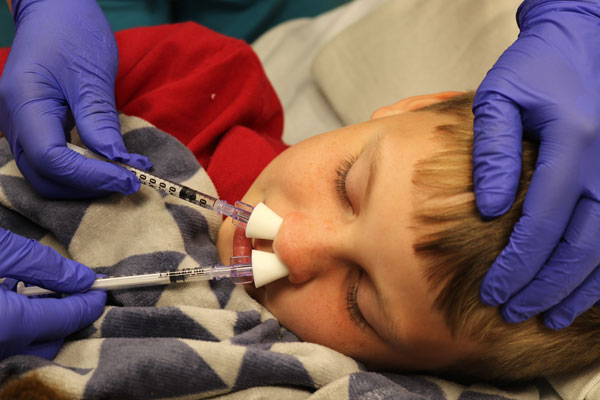
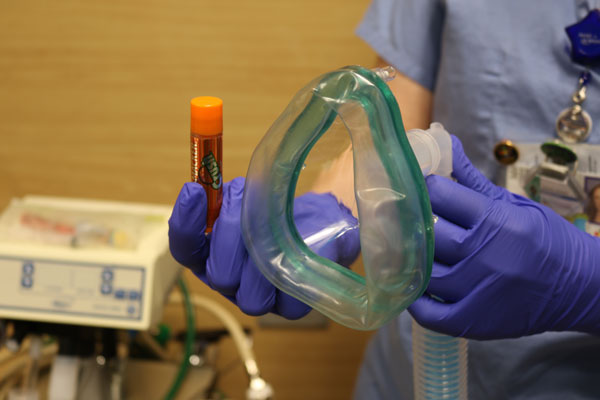
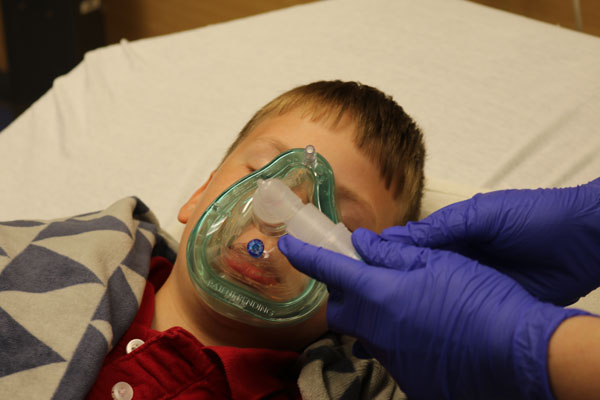
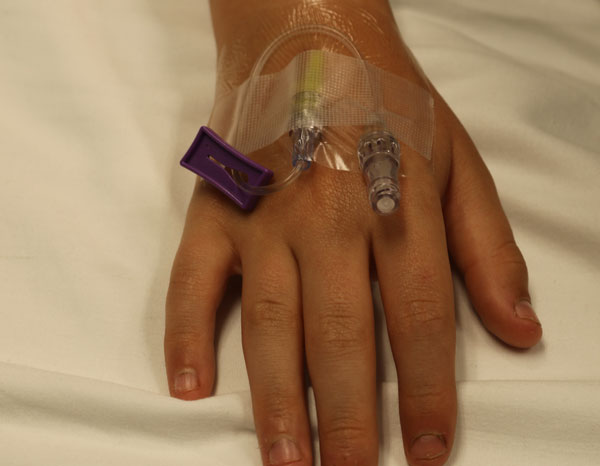
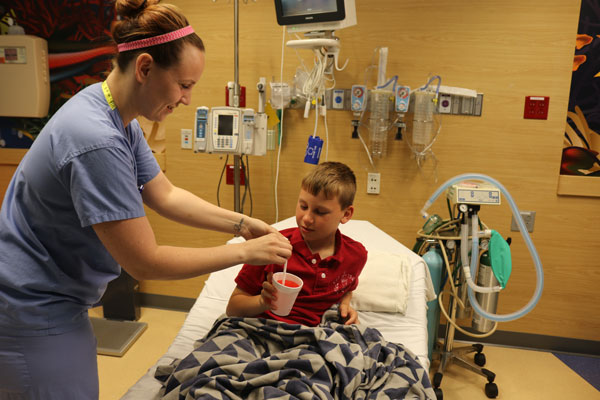

Before Sedation
Morning Prescription Medicines
If your child is on prescribed medications, you may give your child prescription medicine while he or she is still allowed to take clear liquids. Do not give your child medication with apple sauce or pudding. These are considered solid foods. Jell-O can be used as an alternative but only up to two hours before the procedure. Medications that are to be taken later in the day may be given after the child has completed the procedure and recovered from sedation.
Fasting
Sedation requires fasting before the procedure. Our triage nurse will call you several days before your child’s test or procedure to give you specific information about fasting.
The following are some general guidelines:
- Food: Your child should eat no solid foods, including applesauce, pudding, gum or candy, after midnight the evening before the procedure.
- Liquids: Your child can drink clear liquids, including water, apple juice or ginger ale, until four hours before your arrival time.
- Breast milk: Children may have breast milk until 4 hours before the procedure
- Formula: Children may have formula until six hours before your child’s arrival time. Do not add cereal. Do not use formula that has cereal already added.
- Avoid brushing teeth or chewing gum as either will stimulate your child’s stomach secretions. Please be sure there are no snacks left in or around your child’s car seat.
Note: Orange juice is not considered a clear fluid.

What to Bring
To make sedation as easy as possible for you and your child, please bring anything you think will be comforting or entertaining during expected wait times. In addition, please remember to bring any communication systems your child may have. Our staff also wants to know of any ways we can support you and your child, so please tell us about your child’s likes and dislikes, concerns and needs.
Some suggestions that have worked for other patients and families:
- Favorite book
- Favorite toy
- Favorite “snuggly” item (such as a blanket, binky/pacifier, doll or stuffed animal)
- Favorite cup (if your child has a preferred cup)
- Communication device, if your child uses one.
- Activities to keep your child busy independently (such as puzzles, handheld devices and coloring books)
- Sensory objects that are soothing for your child (such as squishy balls, teething/biting toys and sound-minimizing headphones)
- A drink for after the procedure is complete if your child has specific preferences
On Appointment Day
We are located on the ground floor of Connecticut Children’s Medical Center in 1G. Valet parking is available at the front of the hospital. A typical visit to Connecticut Children’s Sedation Unit typically lasts a minimum of two to three hours. This includes registration, the procedure and recovery.
Please arrive 1 hour (60 minutes) before your child’s scheduled procedure. Our team needs this time to:
- Complete the insurance registration.
- Provide time for your child to be examined by a nurse and doctor.
- Have medications ordered and double checked.
- Have the sedation pre-medication take effect.
- Allow for the IV catheter to be placed if needed.
Most procedures last approximately 30 to 60 minutes. Your nurse will be able to provide a time frame for you depending on your child’s procedure. Recovery will also last approximately one hour. However, each child is different, and some children wake earlier while others require longer recovery times. We suggest siblings stay at home to minimize distraction. If this is not possible, please bring toys, coloring books and favorite snacks to keep children entertained. After registration, one of our staff members will guide you and your child to an assigned sedation room. This staff member will measure your child’s weight and vital signs (heart rate, blood pressure, oxygen saturation and temperature). A registered nurse (RN) will join you and will go over the sedation process with you. A physician will examine your child before sedation begins. They will also ask for your written consent for the procedure. A Child Life Specialist will help prepare your child for his medical procedure by using age-appropriate education and supportive activities. A Child Life Specialist is a professional trained to speak with children about the procedure.
After Sedation
Ask to be present before your child wakes from sedation, if allowed. When medically cleared, offer a preferred snack that has been approved by staff. Bring this item from home. Once your child is ready to leave, the nurse will give you instructions on how to care for your child at home. The nurse will also give you a number to call for any questions or concerns that arise after you go home. Some things to keep in mind:
- Many children can have side effects from the sedation medication for up to 24 hours after their procedure. Be aware that they may be sleepy for several hours, they may have vomiting, and they may have some difficulty with balance.
- Some children also have challenging behaviors for a few hours after sedation.
- Some children may need to stay home from school the next day, so a plan should be in place just in case.
- Wheelchairs are available to get your child back to your car once you are discharged. Feel free to bring a stroller if your child is small.
- For your ride home, we discourage public transportation (bus or train) for the following reasons: your child may vomit, and your child may require mild confinement to maintain her safety. A car seat or seatbelt is ideal.