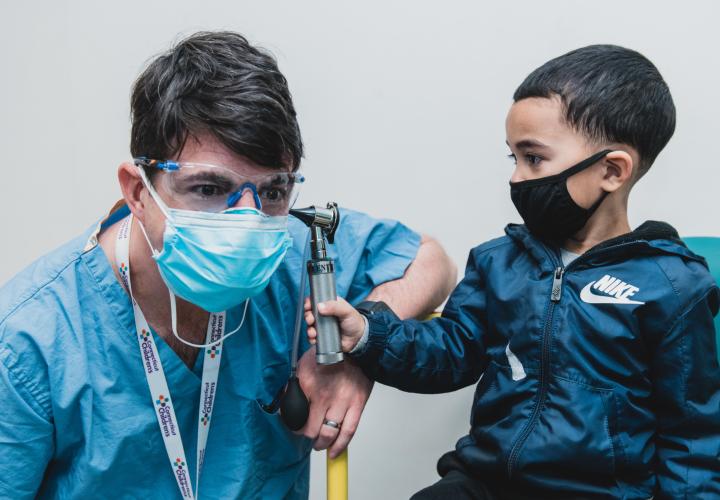
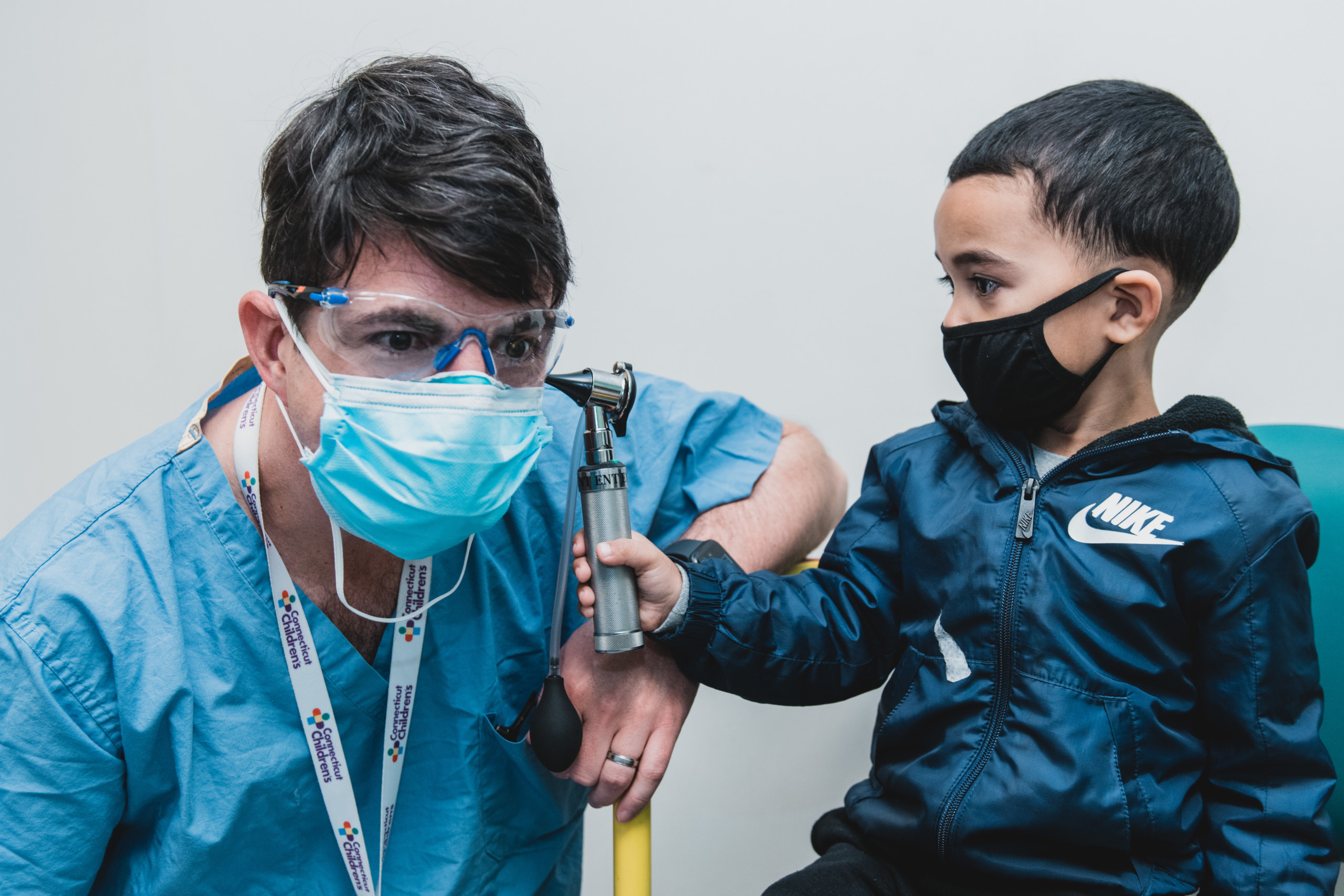
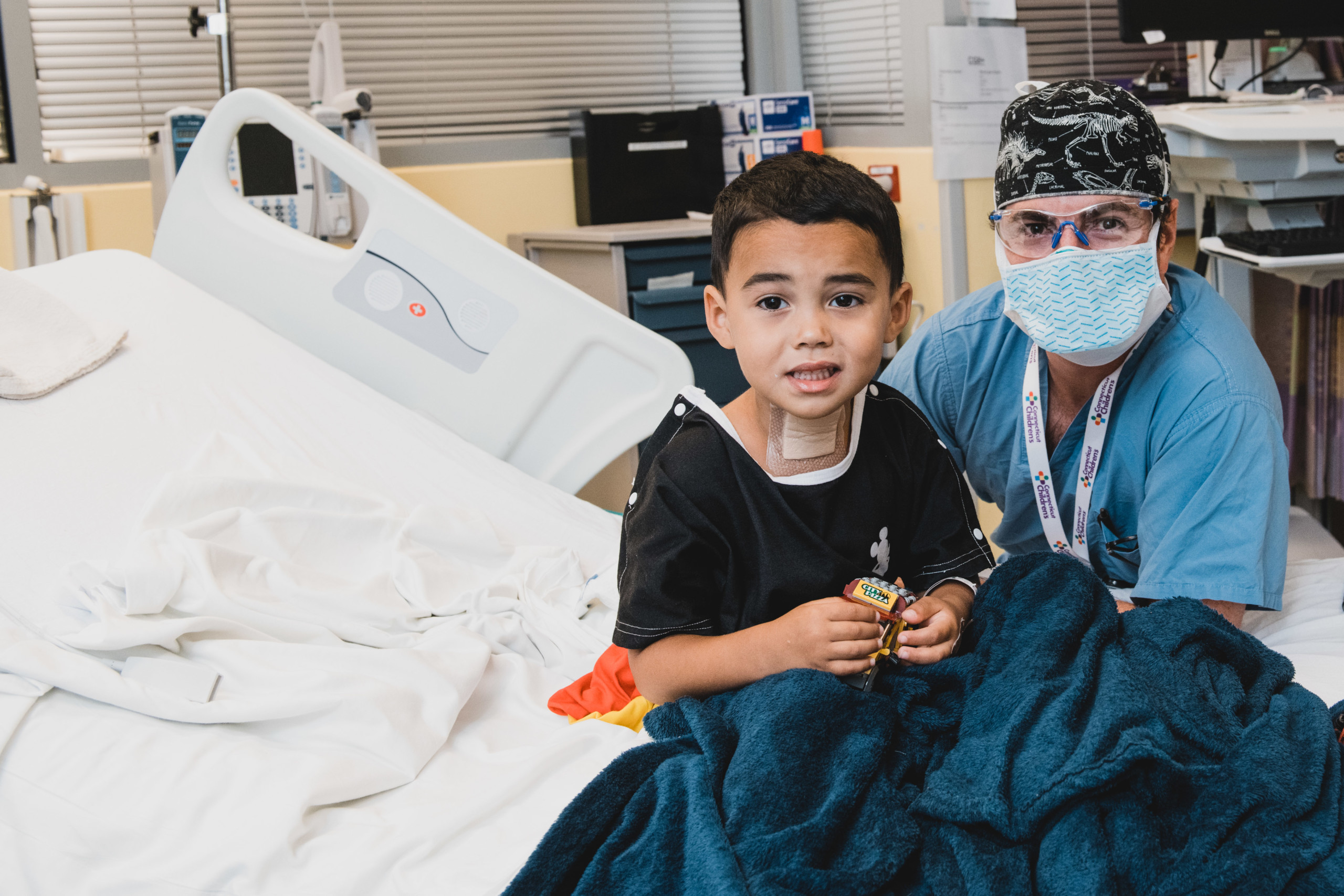
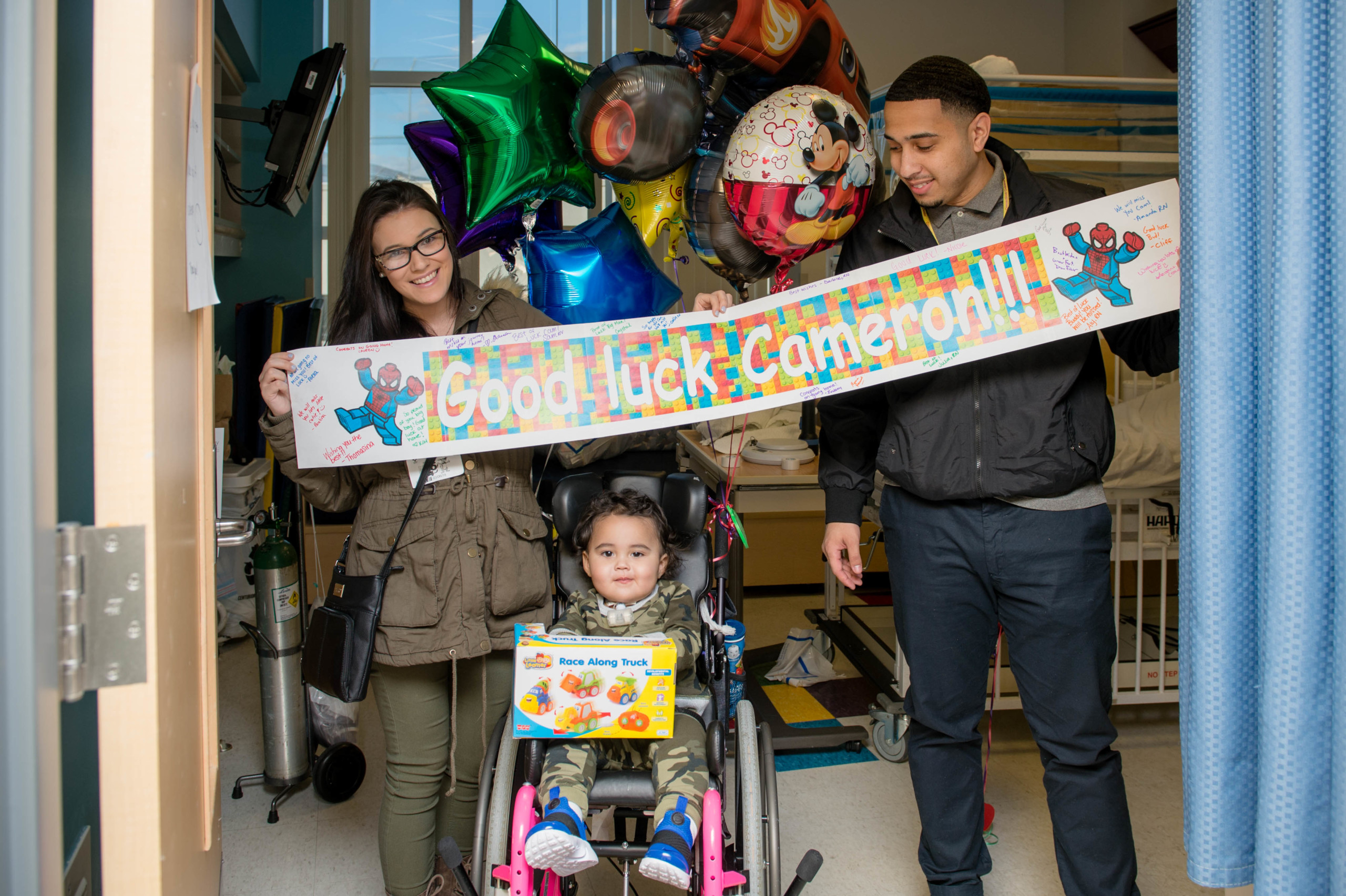When Cameron Soto had a life-threatening injury three years ago, a highly specialized team saved his life. Surgical innovation transformed his future. And compassionate care got him through it all.
But if you met Cameron today, you couldn’t know any of that. You’d just see a sweet, chatty 4-year-old with bubbling-over enthusiasm, who has a way of greeting everyone like a friend – and finding common ground in Buzz Lightyear, breakfast, and assorted superheroes. You’d see a kind, healthy kid who is constantly making his corner of the world a better place.
“He is making up for lost time,” says mom Marisa.